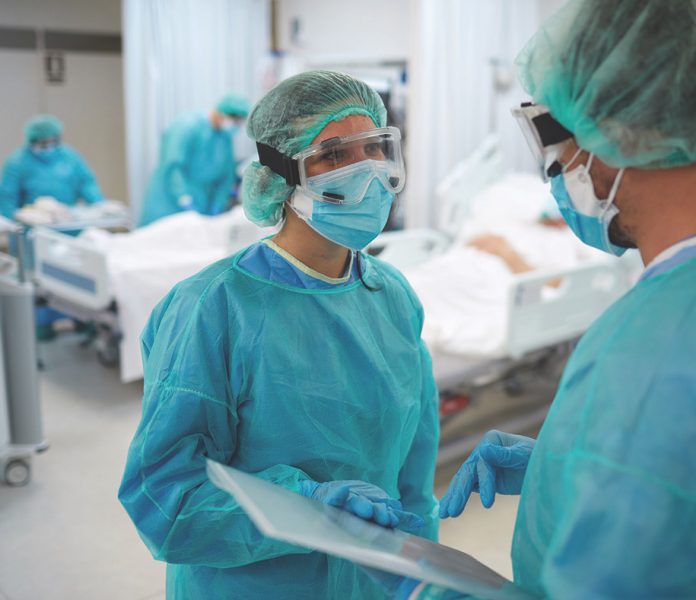
Across the country, one year later, more than 29 million have been infected and there are more than 500,000 deaths due to COVID-19. Here in San Diego County, doctors, nurses and staff at local hospitals on the frontline of combatting the COVID-19 pandemic, look at lessons learned over the past year with the COVID-19 pandemic locally, and what they hope to see in the upcoming year.

Sharp Grossmont Hospital Chief Medical Officer Nancy Greengold, MD, MBA
Sharp Grossmont Hospital Chief Medical Officer Nancy Greengold, MD, MBA, said at the beginning of the pandemic, they were just feeling their way and did not think they had a full sense of how challenging facing COVID-19 would be.
“We could only guess how rapidly the virus would spread, the various mechanisms by which it was spread, or how best to try to treat it,” said Greengold. “Everything was new, from what type of personal protective equipment we needed to lab testing to management recommendations.”
Greengold said Sharp was accustomed to dealing with operational challenges in a busy hospital and has extremely experienced disaster management teams.
“However, this particular crisis has been much tougher than anything that most modern-day hospitals have faced in that it presented a threat to everybody, not just a subset of humanity. Information about how COVID is transmitted grew quickly, forcing us to evolve our practices fast, especially in relation to infection control, the use of personal protective equipment, and laboratory testing,” said Greengold.
Marguerite Paradis, director of Emergency Care and Critical Services Sharp Grossmont Hospital said in the beginning, as a nurse, like everyone else in healthcare they were watching what was happening on the other side of the world. She said looking at the images of overwhelmed hospitals, refrigerator trucks for the dead, she wondered if local hospitals would see this being a first world country and be able to manage it, or if it would be the same here.
“I was watching it and thinking about how this would impact us,” said Paradis. “I remember watching the news. We were screening, but it was before we were even taking precautions. Everyone coming into the hospital was considered exposed or having COVID-19. Even before that, I remember it being very surreal. Was this really going to come?”
Paradis said Grossmont has an astute emergence preparedness team, had done a lot of work around Ebola, so they were prepared for some of the most contagious diseases out there.
“This is a very contagious disease,” said Paradis. “It could strike a large portion of the population and have a detrimental effect on people having profoundly serious symptoms. Death was one of those outcomes for many people. We did not understand at the time what it was going to be like, but that was sort of our frame of reference. I remember when we were meeting, we thought we would need to utilize some of those concepts as Ebola.”

Scripps Mercy Hospital Chula Vista Physician Chief Operations Executive Dr. Juan Manuel Tovar
Scripps Mercy Hospital Chula Vista Physician Chief Operations Executive Dr. Juan Manuel Tovar said when COVID-19 began heating up in China, then hit the U.S. East Coast hard, there was a lot of concern, mostly because of the unknown. It was a novel virus, new, and few people were studying it, and no one knew how bad it could get.
“At a personal level as a site, how is this going to affect myself, my family, the community?” said Tovar. “There was a lot of fear of the unknown mostly. After the first patient we realized that it was all about needing to adapt to work together as a team and we started the learning process of how to deal with this. Just like people feel prior to battle, as soon as you engage in battle it becomes how do we learn from this, where to do need to go from here, how to best treat our patients, and how to keep ourselves safe.”
Tovar said the best thing that happened at Scripps, was preparing for the virus appropriately. He said its command structure worked so everything was in step operationally. Scripps has five hospitals in the region, so leader from all facilities from around the county came together, collaborated and shared information.
“The importance and benefit of that, if you recall the scenes from back east and Los Angeles, there were hospitals that became so full that suddenly you are getting patients in hallways, refrigerated trucks outside because they just reached their limit and people were dying left and right,” said Tovar.
Tovar said there was communication back and forth, the needs were identified, they did tabletop exercises anticipating the flow and the number of patients they were going to get, what happened when they exceeded certain metrics and benchmarks, and where to go next.
“We met virtually on a weekly and sometimes a biweekly basis with leadership,” said Tovar. “We exchanged a lot of information. Anything that came up was directed and addressed and that was how we were able to quickly learn from what we were seeing on the ground and making sure the treatments needed on the ground were available.”
Tovar said they made sure the proper PPE was available, the supply chain, when something was needed, they worked to make sure it was there just in time.
“That really made it manageable,” said Tovar. “A once in a lifetime generational health crisis, we were able to handle it as best we could and made sure we brought attention and treatment to the patients in our community.”
Paradis said as more information came out about COVID being an airborne transmission, there was a lot of conflicting information on how to keep yourself safe, what PPE to use, so they continued to prepare and began screening patients. But she said the criteria of suspected COVID cases evolved as well.
“Anyone traveling from other regions we isolated and started preparing other areas in the hospital where those patients could be seen separately, because we knew it was a highly transmissible illness,” said Paradis.
Paradis said people at the frontline began using PPE because they were screening patients, but once screened, very few met that criteria. As it evolved and became more prevalent, everyone in the hospital began wearing PPE, depending on what the risks were at that time, especial those looking at symptomatic patients.
“When this first started, we were not getting results back right away,” said Paradis. “It would take five to seven days, sometimes longer, so everyone that came in with that criteria and were suspected of having COVID, you waited until those results came back. In the beginning, most of them came back negative. We were still in the midst of the flu season, so we were going back and forth because the symptoms overlapped. Many patients were isolated waiting for results, some came back positive, some negative. We had patients come in that were really sick, acutely ill, and sometimes they did not survive. If they did not survive, they would pass away before we even got results. So, we did not even know some of those patients were actually COVID but had COVID symptoms.”
Paradis said that if it took five to seven days for results now, there is no way the hospital could have managed the population of people that were symptomatic and ill coming into the hospital. She said Grossmont is a remarkably busy hospital and had done emergency trials on managing patients that needed isolation. She said looking back, she thinks that Grossmont did an amazing job.
“We met daily. We had an incident command structure in place with six incident commanders. We were the holders of all of the knowledge and information,” said Paradis. “Anything that come through the hospital came through us and we disseminated the most recent information. It made it so that when we gave out information, it was the same information. It did not come from different areas. So, the emergency department, the inpatient areas, everyone was getting the same information at the same time.”
Paradis said that it was the structure on how information was disseminated to COVID nurses and leads, that helped determine how to manage patients, both COVID and non-COVID. Everyone was informed of new processes at the same time in the emergency department, ICUs, and all other areas of the hospital.
“There was a lot of back and forth, and sometimes in the same day you were updating processes like how we were doing swabs, how we were incubating people, what kind of PPE we were wearing, what was considered more exposure, what were the highest risks procedures,” said Paradis. “All of that was coming in in that first month, but what was considered high risk or low risk, how we were going to mitigate the risks was changing all of the time. Incident commanders met twice a day and our incident command structure was open 24/7 from the very beginning.”
Paradis said my early March, the hospital began its incident command structure. There is an incident command commander, an incident command structure and an incident command center. Paradis said anyone who needed clarification could call the incident command number 24/7 and get answers.
“It was a lot of work and we worked endlessly,” said Paradis. “I was working 16-hour days. Sometimes you would work the day, go home to sleep and come back at the night shift because there were only six of us that were incident commanders. We rotated so we ran the command centers, not adding new people because they would have to be brought up back to speed. We are still the same six incident commanders. For the last year, 24/7, somebody has been at the incident command center or on call.”
Greengold said when COVID-19 patients were at the highest levels, there were many challenges, but one of the largest was trying to communicate effectively with families who were not allowed to be in the hospital.
“The rules against visitors have been terribly hard on patients, families, and healthcare professionals alike,” said Greengold. “Trying to have sensitive conversations via phone or video requires compassion and understanding on both sides.”
Greengold said the teamwork at Sharp has been spectacular and she believes many people have grown closer at work.
“But it has been traumatic for them to see so many patients die, particularly without their loved ones allowed at the bedside,” said Greengold. “Also, professionals are affected not only in their work lives but also off-duty, as individuals grappling with their own fears, sense of isolation, and worries about loved ones. I do not think we yet fully appreciate the long-term psychological effects this experience has had on people working in healthcare.”
Tovar said load balancing between facilities was crucial in keeping the entire system from becoming overwhelmed.
“They were able to take care of those patients there and at the same time we were able to maintain our capacity and also our ability to see people and treat them appropriately without having to cut any corners or be without machines because the system was able to absorb these patients,” said Tovar. “During the height of the pandemic, the human toll, and I am not just talking about physicians and nurses, but our community was being ravaged by this. We saw a lot of extremely sick patients over a long period of time. It has been a year now and these patients take a long time.”
Tovar said the average length of stay in a hospital is four to five days. COVID-19 took up to nine to 12 days average. There were patients that stayed in Scripps hospitals from 40 to 60 days.
“The physical demand because of the intensive work, the patients, the stress, and the fact that you could not get family members in there because the family was at risk at getting ill because COVID is all around them,” said Tovar. “Nurses, physicians, and providers became the extended family. A link between the actual physical family of the patient and the patient. All of that was quite emotional.”
Paradis said the hardest thing for nurses to deal with was the lack of family and the ability of visitations for patients. She said this pertained to COVID and non-COVID patients. Some visitors were allowed for end of life early on, but for COVID patients, absolutely no visitors were allowed.
“It was very difficult initially,” said Paradis. “These patients were being diagnosed with cancer, emergency surgeries. Every possible scenario of what patients experienced, continued to happen and they could not have family there. They were getting results of their tests and could not have family with them. When I think about it, it was extremely devastating to the staff.”
Paradis said Grossmont is an acute hospital and saw many patients who did not require admission, elective procedures were not being done, so during surge times the patients admitted were very highly acute or in some type of recovery, still with the inability to see family or friends. She said some patients could face time and communicate on their own. The hospital set up the ability to hold Zoom meeting with families in every department and set up an area at the hospital to perform Zoom meetings for those who did not have access from home. She said though she was thankful that this could be done, it was exceedingly difficult for staff treating patients.
“The COVID patients, the really sick patients that were incubated or using non-invasive breathing machines, they could not have visitors because they were the highest risk patients because they were using aerosolizing procedures,” said Paradis. “If you were on a ventilator, it was an extremely high risk, so we did not allow families in the room. Those patients that did not survive did not have families coming in. There was a lot of fear from families, even if they wanted to come in, trying to explain to them the transmission and why it was so difficult for them not to come in, they were devastated.”
Paradis said initially, staff feared being exposed to patients, but as time went on and dealing with the patients and families, that fear turned to sorrow.
“Being so impacted dealing with families that could not come in and patients that had to be alone,” said Paradis. “They were the only person that was with that patient at the time of death. It is tremendous. There are lots of tears in the ICUs and COVID units. Lots of support between the nurses.”
Paradis said COVID patients are placed in a negative pressure room, the doors are closed, there are monitors so you can hear the alarms, IV poles are outside the rooms, so nurses are doing a lot of treatment and giving medications outside of the room. Paradis said this is necessary with COVID, because of its aerosolizing transmission it hangs in the air much longer than droplets, that do not require negative pressure rooms.
“When you have to go inside the room you are trying to think about everything that you can do while you are going inside,” said Paradis. “You have to put on a hood, a negative pressure machine and don all of the PPE. You must be very strategic about when you are going into the room. That is what it is like in the day in the life. When you do go in, spend that time with that patient and get everything done because you know you will not be able to go back in for a while because you will take off all your PPE, and it would take you another 20 minutes to get back into your PPE before going back in.”
Paradis said one of the most surreal moments was when the hospital was so full holding 50 to 60 patients in the emergency department and eight or nine patients in ICU.
“I just did not know if it was going to continue and what we were going to do if it did,” she said.
Paradis said they managed the surges because they opened all available rooms, expanded its ICU capacity to accommodate the constant inflow of patients.
“Getting the call that there were that many patients waiting and not knowing for sure if we could accommodate if the surge continued,” said Paradis. “Even though the surge continued, and we managed, that was the most surreal moment for me. We always had enough PPE, good resources. Initially, the overwhelming amount of information coming in, this was all manageable. But in the height of the surge, was it the peak of the surge for me or was this just going to go on and continue to go up. Is it going to continue to grow and start having patients in the auditorium? Was it at the point to where we were putting patients in non-patient areas? Those were the biggest questions.”
Paradis said before San Diego had its largest surge, and New Orleans was being hit hard by the pandemic, she read an article from a doctor there about a young 20 something year old man that was in a car accident, coming into his hospital with a broken humerus.
“I’ll never forget it,” said Paradis. “He went to do an x-ray of the shoulder and he caught a piece of the guy’s lung. The x-ray had the ground glass look like COVID. This was a young fellow, perfectly healthy, in a car accident and had no COVID symptoms. It prompted the doctor to do a chest x-ray and sure enough this young guy had full COVID lungs. He had no symptoms. I still remember ready that and thinking what is happening. What is going on?”
Paradis said there are asymptomatic people that have damage to their lungs and do not even know.
“And truly, that is what happen,” said Paradis. “People can have COVID and be completely asymptomatic. Usually, you have something. That made me think, ‘oh my goodness, what is going to happen? What does the future of this hold?’”
Tovar said Scripps has been wonderful in providing for our physicians and staff with mindfulness classes, music therapy, peer programs where peers can talk with each other and relate and share their what they are feeling. All that to make sure that they keep people as healthy as possible, both physically and emotionally.
Paradis said the hospital set up quiet rooms and healing rooms, and there was a lot of support that staff could go to, and this continues today.
“As much as we are not seeing the surge right now, we still have many COVID patients in the hospital,” said Paradis. “It has decreased in volume, but the actual course that a patient that is deteriorating with the worst of COVID illness are still in the ICUs. We are hoping that this will change for non-COVID patients in a little while because the risks are changing, but right now the visitation has not changed.”
Greengold said along with many counties, San Diego had major challenges during the late fall and early winter, when it saw its highest hospitalization rates for people with COVID and its ICUs were at capacity.
“Death rates also increased in counties across the country,” said Greengold. “San Diego County has been having death rates lower than some counties and higher than others.”
Greengold said obviously, no one has a crystal ball, but she does worry about the present variants, which are thought to be more infectious and possibly more aggressive than the original coronavirus.
“The good news is that scientists are working on more vaccines and boosters to address the variants, which should be able to slow transmission,” said Greengold. “But in the meantime, we can expect more mutations, leading to new variants because viruses mutate. The key thing is that they have more of a chance to mutate when the numbers of infections are surging. So, while the level of virus is still high in society, which it continues to be, we need people to do their part by wearing masks and social distancing. By helping control the spread of the virus, people can slow down the mutation process that creates new variants. We are in a time crunch: we need to lower the level of infection fast, while we continue to vaccinate, so that we can catch up to the current set of viruses. I am concerned that not enough individuals will have the patience to get us where we need to be.”
Greengold said the short-term information about COVID-19 vaccines makes her feel optimistic about their effectiveness. She said that she does think it is likely that boosters will be needed in the future and is encouraged that the vaccine manufacturers are already working on these. Greengold said she does believe that it is possible to attain herd immunity if enough people get vaccinated.
“Vaccination, coupled with the fact that a lot of people have been infected with COVID, symptomatically and asymptomatically, will help us reach herd immunity,” said Greengold.
Greengold said her biggest hope in the upcoming year is that the production of vaccines continues to ramp up and that everyone that is willing gets vaccinated.
“And not just people in the US, but people throughout the world since this is a virus without borders,” said Greengold. “My biggest fear is that many people will shy away from vaccines out of fear or ignorance. If there are not enough people accept the vaccine, the virus will continue to mutate and we will fall behind the curve, even while continually developing new vaccines and boosters.”
Paradis said looking at the year ahead, she is not letting her guard down because there are new variants to COVID, and she believes a surge could happen at a moment. She said that is in the back of the minds of everyone and hopefully this does not happen.
“Last year when they told us we would see the surge in June and another in August, it really did not happen that way,” said Paradis. “I would not bet all my money on another huge surge coming, but I feel that until everyone is vaccinated or until we know the variants will not overcome people with the vaccines. We are planning appropriately because we are now seeing less patients, but I do not think any of us are thinking that we can close shop. We are not at that point yet.”
Paradis said there is a pool of people that do not want to take the vaccine. She said she used to not worry as much about people that were anti-vaccine, but that there have been outbreaks of pertussis, a mix of measles.
“Though I so not know the percentage of people that will not get the vaccine, I think there is the possibility of smaller surges,” said Paradis. “I do not think that we may see the surges that we just came through, but I am hopeful. I just do not know. I do not want to get my hopes up too high or put down my guard.”
Tovar said with new variants surfacing, the problem is twofold. His concern is people will drop their guard now and become infected. He said looking at the research, the vaccines are quite effective, but you must get vaccinated for it to work.
“Get vaccinated because it is going to help you, but also, you have to keep doing what we have been told to do,” said Tovar. “You have to wear a mask, you have to wash your hands, and you have to socially distance. It is a cause for concern that we have these variants. But the good thing is that the science is showing us that if you are vaccinated, it helps you. As a society, we were able to invest in companies that were able to get us these vaccines so quickly, I am quite sure that they are going to be flexible and react. What we need to do is to make sure we continue to do what we have been doing. It is proven that these steps help control the amount of transmission. Decreasing the amount of transmission will decrease the number of variants.”
Tovar said we are now seeing a decline in cases, society is beginning to open, however, this is a fragile moment.
“You think maybe we are at seeing light at the end of the tunnel and we are out of this,” said Tovar. “We may be, and some might say ‘Let’s party.’ But if we drop our guard, not wear masks, start gathering in groups, party, getting back with best friends, close contact, that is going to create an environment for these new variants to take hold and become dominate, and spread quickly through our community. This will hurt our elders, people that have comorbidity, and those with underlying conditions. Some of them could be family. We just need to be careful. We need to continue to slow the spread and make sure that any mutations that occur are not going to become the dominant ones.”
Tovar said although it is still early, he is happy how fast the vaccines came out and their results. He said he has a high degree of confidence that they are effective. He also said, he was happy to see at Scripps, that vaccination was an “all hands onboard” approach.
“We did not just give it to the doctors,” said Tovar. “From the person who does the cleaning, environmental services, to the respiratory therapists. We knew that we needed to treat the whole. If you do not treat the whole, there will be gaps, ways for the virus to continue. People are going to get sick. Everybody is important. And everyone that works in the hospital is at risk.”
Tovar said he believes we are doing well and that the country will meet the metric of 100 million in 100 days with vaccines.
“Scientists say herd immunity is at 72% of the community,” said Tovar. “That is not only those that have been vaccinated, but also the number of people that have had COVID. I think that the vaccines are going to put an end to this pandemic. I am fully a proponent of getting vaccinated. It helps you. It helps our community. It is part of being a good citizen. The government is buying more. More of it is coming to our community, and there are superstations out there to get your vaccine. I you are offered the vaccine, then I say sign up and get that. It will help you, your family, and it will help the possibility of you not getting a harsh or deadly case of COVID-19. You are still at risk of getting it if you are not careful.”
Tovar said his biggest hope is that people realize that we are all in this together, and everyone must do their part, and that everyone remains vigilant.
“Because if we are, do not let down our guard we can let the vaccines do its work. This virus will go down and we will get to some since of normal,” said Tovar. “I want people to realize that our new normal is to be careful. Going back to normal like we were before COVID might not be able to happen. You just have to be smart about it.”
Paradis said though she is sure it is the same at all the hospitals, when she looks back, she admires how Grossmont’s entire team stepped up and remained flexible.
“As the volume increased, we had to open new COVID units, then more COVID came in and we would have to go to a department and tell them they had to become a COVID unit, we need more COVID beds,” said Paradis. “We had no push back at all at the hospital. We used every bed that was possibly available, and everybody just did it. It makes me so proud that we came through this and were able to be so flexible and move with whatever happened. We never countered any resistance, and it makes me so proud of the entire hospital staff. The entire hospital just did what they had to do. It just happened.”
Tovar said Scripps Mercy Chula Vista has been in this community an exceptionally long time and if there is anything he could say about the hospital, is that it is resilient.
“We get knocked down, we get up and we keep going,” said Tovar. “We support each other, and we love this community. I have worked in this hospital more than 20 years and I would not work any place else. This is a great community. It has a diversity of cultures, backgrounds, and the people are the salt of the earth. Everybody that works in this hospital works here because we love it. We love coming here and being part of this community.”
Tovar said although he is sure this is the case around the county, the staff at Scripps appreciates how the community supported them. He said they received, food, supplies, cards from school children, and much more.
“Emotionally it was really tense, but also at times really gratifying and uplifting. This balance kept staff going,” said Tovar. “We are so grateful to the community for their support. It was heartfelt how the people rallied around us. We might not be able to answer them, or say thank you on a personal level, but they should know that we would not be anywhere without this community. This is a particularly important community to Scripps, and we want our community to thrive, continue to grow, and be healthy.”
Tovar said this country is amazing and it has done so many great things throughout history.
“This is going to be one of those things,” said Tovar. “We come out of this. We learn, and we are better for it. I am very hopeful for our future and I know we will beat this pandemic. Scripps and the other health institutions in the region will help keep you safe and to be part of the solution.”